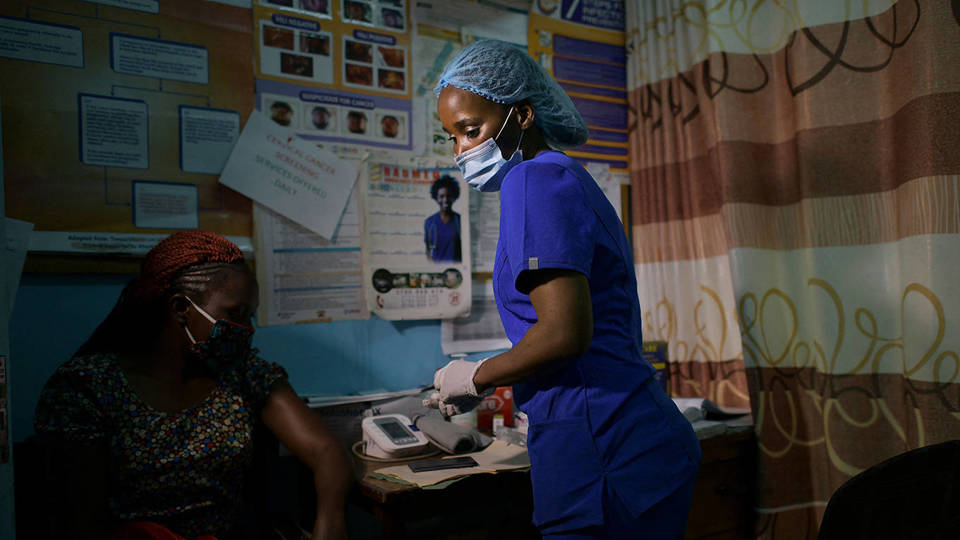
 Tony Karumba/AFP via Getty Images
Tony Karumba/AFP via Getty Images
en English
Walter O. Ochieng and Tom Achoki
Rather than address the weaknesses of the grant-based approach to global health financing, donors want to scrap it in favor of instruments that mobilize more private capital. But this new architecture distorts the risk landscape in ways that socialize losses, while privatizing profits and control.
Once you get past the jargon, however, it becomes clear that this new architecture distorts the risk landscape in ways that socialize losses, while privatizing profits and control. Of course, altering the distribution of risk is the point. For example, guarantees entail an entity (usually public or philanthropic) pledging to step in if a borrower defaults on a loan from private investors. Enabling private actors to enjoy financial and reputational benefits, with capped downside risks, lowers the cost of capital for projects deemed socially valuable.
But the results are far from benign. Donors claim fiscal prudence, but they are committing to obligations that materialize when things go wrong. Since the shocks that are covered – such as currency depreciation, political instability, regulatory changes, and weak demand – are very common in lower-income countries, the chances donors will have to pay up are high. Recipient governments, meanwhile, remain bound by their repayment obligations, often denominated in foreign currency.

Get three months of PS for $1
Read all the newest insights from the leading and emerging voices shaping global debates with a PS trial subscription – just $1 for three months.
Try PS for $1
Consider vaccine manufacturing. Guarantees can de-risk factories and encourage local production – a genuine public good, particularly in a region Africa, which imports over 99% of its vaccines. But vaccine demand is volatile; procurement depends heavily on donors; and margins are thin. To make projects bankable, guarantees often extend beyond construction costs to cover offtake risk or exchange-rate losses for years. When vaccine demand collapsed after the COVID-19 pandemic, manufacturers’ liabilities did not disappear; they shifted to the public actors that had underwritten the risk.
This redistribution of risk affects decision-making. Private actors have little incentive to exercise discipline when they know their losses are backstopped. And risk-laden guarantors are more ly to emphasize the financial viability of projects, rather than the health system’s needs. Revenue-generating services (urban hospitals, diagnostics, tertiary care) are favored over lower-margin investments (primary care, worker salaries, rural clinics) that offer the most cost-effective health gains. Most of the private health investment that development-finance institutions have mobilized in low-income countries has gone toward hospitals and specialized facilities.
Guarantees flatter the technocratic belief that the main constraint on global health is money – and, specifically, the structure of financing. But the biggest constraint is politics, in both donor and recipient countries. Guarantees cannot conjure sustainable health financing where tax bases are weak, debt burdens are high, and trust in public institutions is low. Low-income countries now spend more on servicing external debt than on public health – a constraint that no amount of leverage can overcome.
Furthermore, guarantees cannot change the domestic political economy. Governments underinvest in health even when capital is accessible, because health spending delivers diffuse benefits, whereas other priorities – security, patronage, and visible infrastructure – offer more concentrated political returns. Nor can guarantees deliver the long-term recurrent spending – including on personnel, maintenance, and logistics – that is needed to keep a health system running. Private capital diss overhead and operating expenses; it prefers assets, contracts, and exits.
This is not to say that guarantees have no place in global health. But they should be used sparingly, transparently, and for genuine public goods, such as pandemic preparedness, regional manufacturing capacity, or cross-border surveillance systems. And they should be evaluated not by how much private capital they mobilize, but by whether they strengthen health systems without shifting unsustainable risks onto fragile governments.
Meanwhile, donors must honor existing grant commitments and increase overall ODA. And efforts must be made to support domestic resource mobilization in low- and middle-income countries, such as by strengthening tax systems and improving governance.
Global health does not suffer from a lack of clever financial instruments. It suffers from a shortage of predictable funding to pay nurses, keep clinics open, and ensure that drugs arrive on time. The language of leverage might appeal to those who make funding decisions, but it will do little to fix health systems on the ground.
Help us strengthen our reporting on global health and development by taking a short survey.
Take Survey
Featured
-
Trump’s Biggest Energy Bet Isn’t in Venezuela
Jan 27, 2026 Sarah Ladislaw
-
The Coming Crypto Apocalypse
Feb 3, 2026 Nouriel Roubini
-
Markets Are Shrugging Off Uncertainty
Feb 3, 2026 Dambisa Moyo
-
Trump’s War Against the States
Jan 30, 2026 Steven Simon & Jonathan Stevenson
-
What Would a Bardella Presidency Mean For France?
Jan 30, 2026 Brigitte Granville
Walter O. Ochieng
Walter O. Ochieng is a physician and global-health researcher at the Africa Institute for Health Policy.
Tom Achoki
Tom Achoki, a former Sloan fellow at MIT, is a physician and Co-Founder of the Africa Institute for Health Policy.
https://prosyn.org/RtA9CbK
Sumber Artikel:
Project-syndicate.org